North-Central, Niger State: A 22-year-old Rahmatu Mustapha is a resident of Panbe, a remote area in Minna, Niger State, Nigeria. She gave birth to her three children with the help of a midwife in her maternal hometown in Minna, where she always goes to stay whenever she is about to deliver. This is because there is no health centre in her community.
But for the fourth pregnancy, her husband insisted she deliver in Panbe. Mrs Mustapha lives at a 25-minute distance to Beji Primary Health Centre, the nearest facility.
When she was due for delivery early February in 2023, she struggled with labour pains while her husband was up in the middle of the night running around the neighbourhood in a quest to get a vehicle to take her wife to Beji health centre.
“I gave birth to my three children at my mother’s village in Bosso because we don’t have a clinic here in our village, but they have a nurse that assists women with deliveries there.
“My husband objected to me going there to deliver our fourth child. A lot of things happened that we couldn’t get to the hospital in Beji quickly,” she said.
In spite of the progress made in the last few years, maternal mortality cases have been reported increasingly in Nigeria due to the delays and inaccessible healthcare that could have prevented them.
Findings by CISLAC shows that one in 13 women dies during pregnancy and childbirth in Nigeria, many of which would have been prevented if there had been prompt access to healthcare.
In Nigeria, according to the National Bureau of Statistics, the maternal mortality rate presented 576 per 100,000 live births, while the neonatal rate is 39 per 1,000 live births and 70 per 1,000 deaths of infants. The study further shows that one in 15 live births in Nigeria dies before their first birthday while the death of under-five children rate is 120 per 1,000 live births.
In Niger State, one in every 95 women dies during pregnancy and childbirth, amounting to 1,934 annual deaths from pregnancy-related issues.
Halimah Musa, officer-in-charge of Beji health centre said until sometime around 2022, the facility always records low women patronage for delivery.
“Before, delivery in this facility was not much, it used to be 10-15 in one month. Many women engage unskilled attendants during childbirth, ” said Mrs Musa.
The response changing the narratives
Having noticed the delay in accessing and receiving appropriate care by women in rural areas of Niger State during labour, Raise Foundation, a Not-for-Profit Non-Governmental Organisation that facilitates improvement in Maternal and Child Health launched Community-Based Emergency Transport Scheme under its Maternal, Neonatal, and Child Health (MNCH) intervention area to ensure safe delivery for expectant mothers.
The foundation was founded and managed by the wife of the Niger State governor, Amina Abubakar, a gynaecologist and senior doctor in the Neonatal Unit at General Hospital, Minna.
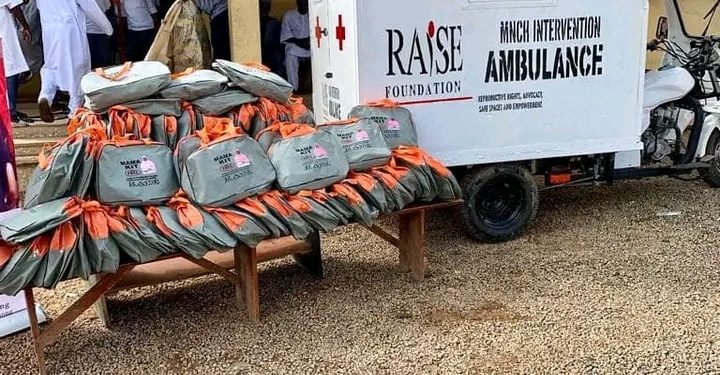
The scheme, with support (periodically) from TY Danjuma Foundation, provides tricycle ambulances for healthcare centres that can manoeuvre through rural terrain areas that are hard to reach.
Ruth Jiya, the foundation’s communication officer said, in 2015, through in-depth interviews with women of reproductive age about their experiences using healthcare services, the foundation conducted an assessment on maternity, neonatal, and child healthcare services across local government areas in the state. It also undertook assessments of over twenty-four healthcare facilities on the quality of maternity and paediatric health services.
“Data were collected from representative households from women groups using focus group discussions. In-depth interviews were conducted with women of reproductive age 15 – 49 and with men ages 15 – 59 in all the sample LGAs. Twenty-four secondary and primary health facilities were assessed for quality of maternal, newborn, child health, and family planning services,” Raise Foundation said on its website.
Mrs Jiya told this reporter that less 50% of women of child bearing age received antenatal and delivery care by skilled providers while others mostly take place at home by unskilled providers. Many secondary health facilities offer less postnatal care while no primary health centres that offer delivery services.
Began in 2017, the tricycle ambulance manoeuvres the rural terrain communities and transports labouring mothers promptly and efficiently for healthcare. The initiative committed to safe delivery for expectant mothers and ensured no woman dies of pregnancy-related issues.
Through the scheme, Mr Mustapha’s effort was applaudable as he was able to find the ambulance contact, which conveyed his wife to Beji health centre after futile efforts to get a vehicle from neighbours.
“My husband met with many people in the village that night to ask for help; everyone was helpless until he found a woman who had the emergency ambulance line of Beji health centre. I was taken there by the ambulance and delivered safely. They also used it to take me back home after I was discharged,” said Mrs Mustapha.
This is a similar story to Sheria Faruq’s, an 18-year-old mother-of-one. The delay she had before getting to the hospital to deliver her first child remains a nightmare she said she would never pray for.
Though her husband has a motorcycle he could use to take his wife to the hospital, it, nonetheless, developed a defect the day before she went into labour.
She attended an antenatal clinic at Beji Health Centre and was provided with an emergency ambulance contact. She was able to contact the centre for help and was taken to the facility and delivered safely.
According to the data obtained from the foundation, over 230 expectant mothers across various local government areas were transported to health facilities to deliver with the help of emergency tricycle ambulances.
The Doko, Lemu, Fuka, and Kabogi Health Centres in the local governments of Lavun, Lemu, Munya, and Mashegu, respectively, are among the facilities that benefited from the intervention which have been filling the huge gap of delay in the life of labour women.
Beyond transport scheme, delivery and immunisation at zero cost
The foundation has also trained health personnel and volunteers working interconnected with health centres and communities to encourage, sensitise and mobilise women on MNCH cares and influence unskilled birth.
Mrs Jiya said the foundation provides totally free delivery for expectant mothers to encourage antenatal clinic attendance and skilled birth. It also provides delivery kits (mama kits) for indigent pregnant women after they attain 70% antenatal clinic attendance at the particular facility.
She said the delivery kits contain essential items required to take delivery by a skilled birth attendant. It also includes instant medications to be taken.
“Everything that is needed for delivery at the hospital is in that our mama kit. We have a preventive dose for PPH, we have pads, jik; that is disinfectant, baby towel, delivery masks, mucus extractor, cord clamp, chlorhexidine;for the cord of the baby and misoprostol tablet that is the drug needed to control bleeding. So everything that a mother needs to deliver in the health facility is in that bag, so you don’t have to pay anything,” said Mrs Jiya.
With this, according to the foundation, over 16,000 mothers and newborns have been supported with delivery kits and medical care within 24 hours of delivery. Newborns are also immunised for free against vaccine-preventable diseases until they turn one.
In an interview with Mrs Musa, one of the beneficiaries of the initiative, said the interventions had improved women’s patronage at her health centre which connects 30 communities.
“With the coming of the interventions by Raise Foundation with ambulance, delivery kits, awareness, outreaches, on-site visits, and sensitization, more women are patronising the facility by attending the ANC (Antenatal Care), and they will also deliver here,” she testified.
The deliveries have increased now, 50 to 60 deliveries are carried out at the end of the month. Mrs Musa said for last month alone, 74 deliveries were taken with the coming of the tricycle ambulance and other interventions.
Doko Primary Health Centre, a facility that connects 13 communities, benefited from the intervention in 2019. Though the centre has a bus ambulance it uses during emergencies, it cannot manoeuvre many terrain areas. Hence, it was provided with a tricycle ambulance to fill the gap for women who stay in the areas.
The officer-in-charge, Sha’ba Baji, while commending the initiative, told this reporter that it has improved newborn deliveries at the centre.
“With the intervention, there has been a lot of improvement in ANC and delivery in our facility.
“During the introduction [of the project] to the communities we gave them our phone numbers, the tricycle, the in-charge office, and myself. Any of them that went through whenever anyone is in labour they just quickly call us if they don’t have any means of mobility.
“We went for training along with tricycle ambulance riders and some women that will be going round to sensitise and give health education to women on antenatal care.” Mr Baji said.
In an interview with Sulayman Taofeeq, the medical director at Dr Amina Abubakar Women Health Centre (Foundation’s health centre) in Kontagora, said the scheme has been preventing labour women from prolonged obstructed labour.
He related the story of a woman in Minna who developed a vesicovaginal fistula due to the delay she had during labour.
“There was a rainfall, her husband was not around and nobody to call. There was actually this delay, she waited, waited, and waited, yet no vehicle to convey her to the hospital, within Minna town! By the time she was taken to the hospital, it was already late. Eventually, she delivered the baby but she already developed a fistula before help came,” Mr Taofeeq said.
“At times, you notice a mother in labour couldn’t get a vehicle to convey her to the health facility, but with this tricycle ambulance, accessibility has improved across areas where we’ve intervened,” he added.

Funding and insecurity limiting the reach
Mrs Jiya, nevertheless, said funding and insecurity were hindering the foundation’s reach.
She said its assessment found that more health facilities need ambulances and adequate maternal and child health care, but the foundation could support few facilities so far due to limited funds.
Mrs Jiya said the support from the TY Foundation for the project had ended and since the foundation has been doing it by itself.
“The project has ended with them, we are just the ones doing it on our own now.
“If we find more money we don’t mind expanding it to more PHCs. It has been an intervention that positively touched the lives of rural women, but you know, finance is the constraint. We’re looking to partner with more international organisations, if we get more funding we will do more.
This story has been made possible by Nigeria Health Watch with support from the Solutions Journalism Network, a nonprofit organization dedicated to rigorous and compelling reporting about responses to social problems.